How to Reorder and Confirm Supplies with 180 Medical
This information was reviewed and updated for accuracy on May 1, 2026.
At 180 Medical, we make the process of restocking your catheters and/or ostomy supplies as easy and stress-free as possible.
Instead of calling in each time you’re ready for a new order, start taking advantage of our automated shipping schedule with these easy reordering options.

3 Easy Ways to Reorder Your Catheter or Ostomy Supplies
We offer several easy ways for our customers to reorder and confirm their upcoming catheter or ostomy supply orders.
1. Reorder with the secure My 180 Medical mobile app or online customer portal.
With the My 180 Medical mobile app for smartphones and tablets, it’s a snap to confirm your supply needs and reorder your next shipment. If you prefer to only access the secure portal on your computer, the My.180Medical portal is an easy option.
With My 180 Medical, you can complete all kinds of tasks without ever having to make a phone call. You can:
- View bills and pay balances
- Make updates to your information
- Get reminders for reordering
- Track shipments
- Complete paperwork
- And more!
Are you a new customer who hasn’t yet registered to access your account online? Just go to the sign-in page at My.180Medical.com and click “Create An Account.” From there, just follow the steps.
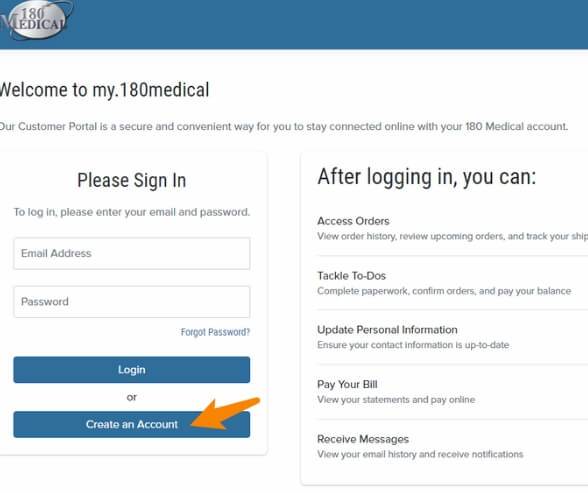
Then you can download the My 180 Medical app from the Apple App Store or Google Play for easy access to your account in just a few taps.
2. Confirm your order by email
If you prefer to avoid a phone call, we understand. That’s why we offer confirmation by email. Just provide 180 Medical with a working email address that you check regularly.
Then we’ll send you an order confirmation email around ten days before your scheduled shipment. Just click the ‘Refill Now’ button, then follow the prompts to:
- Enter the name and date of birth of the customer receiving supplies
- Verify the shipping month
- Let us know whether you are currently receiving home healthcare
- Input the number of supplies you currently have on hand
3. Confirm your upcoming order by phone or text message.
Prefer to talk to someone on the phone to reorder your supplies? We love hearing from you! Or would you rather just get a text when it’s time to confirm your orders? That’s easy too. Just let us know how you’d like to be contacted, and we’ll adjust your account accordingly.
Then our friendly Confirmation Specialists will start reaching out to contact you by phone or text (depending on your preference) you when your order is due to ship soon (typically seven to ten days before your scheduled shipment). We’ll check in with you on how you’re doing on supplies, and at that time, we can go over whether you need to confirm, adjust, or push back your order.
Did you miss a call from 180 Medical’s Confirmation department? Don’t worry. You can bypass the main phone line and reach out to the Confirmation team directly by calling 405-603-8215.
Reordering and Order Confirmation FAQs
Here are a few quick answers to all your common questions about reordering your catheter and ostomy supplies with 180 Medical. For more quick answers about how to manage your 180 Medical account, check out the 180 Medical Help Center!
Why do I need to confirm my order before it ships?
Some insurance providers, including Medicare, Medicare replacement plans, and some state Medicaid programs, require confirmation of the need for the next order before shipping, even when supply needs are recurring.
As a nationally accredited medical supplier, 180 Medical follows these insurance requirements carefully. That’s why, in certain cases, based on your insurance plan’s requirements, we’ll need to get in touch with you to confirm your supply needs before the next shipment can be sent.
This process helps us:
- Make sure you receive the supplies you need
- Confirm whether your supply needs have changed
- Avoid shipping supplies too early or too late so you don’t get overstocked or run out
- Meet insurance requirements
- Reduce the risk of billing conflicts
We know it can feel like an extra step, but we’re here to make this process as easy and convenient as possible. You can confirm your orders in several quick ways, including the My 180 Medical App, the secure online customer portal, or we can reach out to you by phone, email, or text.
Typically, we will call, text, email, or send you a notification about 7 to 10 days before your regularly scheduled order is set to ship from our warehouse. This allows plenty of time for us to get in touch, so you don’t run out or run low. Plus, it ensures that we follow and meet all insurance requirements.
Can I reorder my supplies in person at a 180 Medical location?
We do have physical office locations, but reordering by phone, online, or through the My 180 Medical App is faster and more convenient. These options allow our team to access your account, verify insurance, and process your order without delays. We recommend using these methods instead of visiting a location in person.
What information do you need to reorder and confirm my supply needs?
When we reach out to confirm your order, whether by text, email, phone, or in-app notification (depending on your preference), we may ask a few questions if it is required by your insurance guidelines. Usually, these are the basic questions for customers, although it may vary depending on one’s insurance requirements:
- Are you ready for your next regularly scheduled order?
- How many supplies do you have on hand? (Please note: Effective 1/1/2024, Medicare-insured customers no longer need to count out supplies on hand. You just need to confirm that you do need your supplies.)
- If you have Medicare or a Medicare replacement policy, you may also be asked if you have a Home Health nurse or physical therapist coming to your home, just to ensure there are no billing conflicts.
What if I don’t like phone calls?
You can also confirm your orders by email, text message, or online with the 180 Medical Customer Portal or the My 180 Medical App on your smartphone or tablet.
Depending on your insurance requirements, we may also be able to confirm your orders by text. Just let us know what you prefer, and we’ll adjust your account or help you get started on the app today!
What happens if 180 Medical can’t get in touch with me to confirm my order?
A: We will always make multiple attempts because we know your supplies are important to your health. However, if we are not able to confirm your order, we cannot ship your supplies.
That’s why it’s important to keep us updated when things change, like phone numbers, addresses, travel plans, etc.
If you realize you’ve missed a call or email, just get in touch with us as soon as possible, and we’ll get you taken care of.
Why do you need to know if I am receiving Home Health?
If you’re insured by Medicare or a Medicare replacement policy, we ask for this information to make sure there will be no billing conflicts so that your insurance does not get over-billed. It’s a question that protects you and your insurance.
For instance, if your home health agency bills through Medicare, they are required to supply your catheters or other necessary medical supplies until the end of their services. Once their services have been completed, they must send a discharge summary to us.
But don’t worry. We’ll never leave you hanging. We’ll be sure to keep following up with you and make sure you’re doing okay until you’re ready to resume orders with us.
My supply needs haven’t changed. Can you just ship my orders without contacting me?
We understand regular confirmation of your supplies may seem unnecessary, but we do this to follow insurance guidelines. For catheter or ostomy supplies provided on a recurring basis, billing must be based on prospective rather than retrospective use, so we must contact you prior to refilling your order and not automatically ship on a pre-determined agreement, even if you authorize it.
If you have any other questions, concerns, or changes to make to your account, contact our friendly Confirmation Specialists online or call us toll-free at 1-877-688-2729.
Do I need to count my supplies before confirming an order?
No. Medicare-insured customers no longer need to count out supplies on hand as of January 1, 2024. You only need to confirm that you need your supplies. Other insurance requirements may vary.
Contact 180 Medical for the Supplies You Need
Are you looking for the right catheter and ostomy supply company?
180 Medical provides an unbeatable combination of top-quality products with reliable shipping and personalized customer support.
Fill out this contact form to get started.


