Living with an ostomy means getting really familiar with your body, your stoma, and the skin around it. It’s important to know what a healthy stoma looks like for you (usually moist and pink or red) and recognize when changes like swelling, bleeding, color changes, or leakage might be signs of stoma problems.
Below, we’ll go over some common issues that can affect anyone with a colostomy, urostomy, or ileostomy, including the signs of infection. Plus, we’ll go over some of the early warning signs of tissue death and when to talk to your ostomy nurse or doctor.
What Should a Healthy Stoma Look Like?
Healthy stomas should be somewhat moist and appear pink or pinkish-red. Some compare it to the inside of your cheek.
Keep in mind that the stoma is a delicate part of your body, especially right after surgery. It’s important to care for it gently and keep a close eye on how it’s healing.
A healthy stoma is usually:
- Moist
- Pink or slightly red (like the inside of your mouth along your cheek)
- Surrounded by skin that looks normal
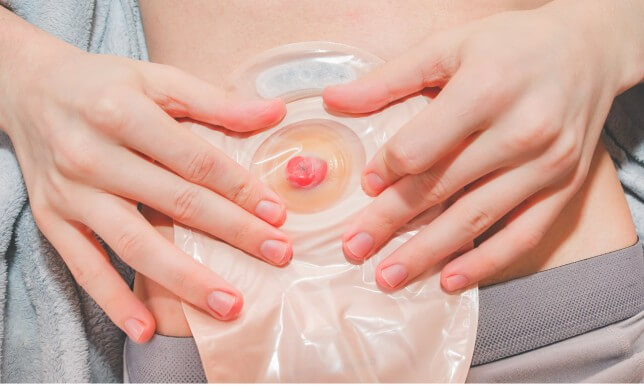
In the first few days after your ostomy surgery, you may notice some swelling or mucus being produced from it. You may want to just stay in touch with your doctor or ostomy nurse if the redness or swelling doesn’t ease up.
If you’re new to using ostomy supplies and dealing with issues like leakage, 180 Medical’s Ostomy Specialists can work with your healthcare provider and insurance to create the right supply order for your needs.
We can also connect you with a team of qualified WOCNs (Wound, Ostomy, and Continence Nurses) who can help and answer questions about your stoma’s health or which products might address issues like pouch leakage, discomfort, or skin irritation from adhesives.
Request Samples to Get Started
What Does an Unhealthy or Infected Stoma Look Like?
It’s important to check your stoma and the skin around it (peristomal skin) regularly. Some changes may be small, like a bit of pinkness after removing your ostomy pouching system. Others, however, can be signs of a stoma problem that needs medical attention quickly.
Signs of an unhealthy stoma may include:
- Appears dry instead of moist
- Color changes like turning pale or going darker, or unusual colors like blue, brown, or black
- Increased swelling or sudden stoma size changes
- Ongoing pain
- Pus-like discharge or bleeding
- Irritation, redness, rash, itching, or raw skin around the stoma
- Retracting inward or protruding farther than usual
- Your pouching system no longer fits well, fits too tightly, rubs, or causes irritation
- Unusual odor unrelated to normal ostomy output
Some stoma problems, like leakage or irritation, may improve with simple changes to your ostomy products or pouching routine, like choosing a different pouch with adhesive that doesn’t irritate your skin or finding a better fit.
However, it’s important to recognize the warning signs of more serious ostomy problems and to contact your doctor, ostomy nurse, or another qualified healthcare professional as soon as possible.
When Should I Call My Doctor or Ostomy Nurse About Stoma Problems?
It’s important to stay in touch with your healthcare professional when you notice changes or anything out of the ordinary.
Contact your healthcare professional when:
- Your stoma is changing to unhealthy colors
- Your stoma is drying out or swelling
- The area around your stoma feels hot, or you have a fever
- You’re experiencing ongoing pain
- You notice pus-like discharge, sores, or bleeding
- Your peristomal skin is red, raw, painful, swollen, or itchy
- Your output becomes unusually watery, suddenly stops, or changes in a way that concerns you
- Your stoma starts to retract inward or protrude outward more than usual
Please seek urgent medical attention right away if your stoma suddenly turns very pale, purple, blue, gray, or black, or if you have rapidly spreading redness, swelling, severe pain, bleeding, fever, chills, nausea, or vomiting.
What Are Some Common Types of Stoma Problems?
Stoma problems can occur for many reasons, including changes in your body, stoma size, output, skin, or how your pouch fits.
Let’s go over a few common stoma problems people with ostomies may encounter.
Peristomal Skin Irritation
The peristomal skin (skin surrounding the stoma) should look like the rest of your normal, healthy skin on your abdomen. However, it’s not uncommon for people with ostomy stomas to experience peristomal skin irritation at some point.
Skin irritation around your stoma can happen for a few different reasons, including:
- Ostomy pouch leakage
- A fit or type of skin barrier that’s not right for your needs
- Adhesive buildup
- Skin stripping from pouch or wafer changes
- Too much pressure from your ostomy pouch system
- Ingrown hairs or folliculitis
- Moisture trapped under the skin barrier
- Allergic reactions
If irritation continues, talk with your healthcare provider or an ostomy nurse. It’s possible that finding a different ostomy wafer or skin barrier size may help.
Certain ostomy accessories are also designed to address common causes of skin irritation, such as adhesive remover wipes, skin barrier wipes, or ostomy seals.
Ostomy Pouch Leakage
One of the most common ostomy problems people experience is pouch leakage.
It can be frustrating, uncomfortable, and stressful. It can also irritate your peristomal skin if output seeps beneath the skin barrier during leaks.
This can happen for many reasons, such as:
- Changes in your stoma size or shape
- A pouching system or ostomy wafer that doesn’t fit well to the curves or contours of your body
- When your pouch becomes too full or heavy
- A skin barrier that loosens quickly
If you’re dealing with pouch leakage, we know it can feel like a constant worry. You might not even want to leave the house. But you shouldn’t have to keep going through it, and there may be product options or other solutions to your routine that can help.
It’s a good idea to contact your ostomy nurse or healthcare provider and let them know about your pouch leakage. They’ll be able to determine whether your pouching system or wafer is the right fit, or whether other issues are causing the leakage.
180 Medical’s Ostomy Specialists can also help you understand your insurance-covered product options, based on your prescription, and we’ll work together with your healthcare provider to find the right supplies for your needs.
Granulomas Around the Stoma
Granulomas are small, raised bumps that can appear on or around the stoma. They’re considered benign, but they can still be irritating or uncomfortable.
They can sometimes interfere with your pouch seal or cause your ostomy wafer to loosen more quickly, leading to leakage.
They may develop over time due to friction or irritation. If you notice new bumps or unusual changes to your stoma, talk to your healthcare professional.
Stoma Prolapse
Stoma prolapse happens when the stoma begins to protrude farther out from the abdomen. It may become noticeably longer over time, which can sometimes interfere with your ostomy pouch seal.
If you notice stoma changes, such as prolapse or an unusual protrusion, get evaluated by your doctor or ostomy nurse. They’ll monitor the size and length of your stoma prolapse and recommend next steps.
Even if it’s not painful, surgery may be needed. However, this isn’t always necessary. Your qualified medical professional will be the best source for advice on what you should do next.
Parastomal Hernia
Ostomy hernias, also called parastomal hernias, can develop due to weaker abdominal muscles. This happens when part of the bowel pushes through the muscles near the stoma. This can create a bulge or unusual swelling just beneath the skin.
A parastomal hernia can be uncomfortable and even painful. They may be more common in people with certain risk factors, which may include, but are not limited to:
- Obesity
- Diabetes
- Smoking tobacco
- Chronic cough or COPD (chronic obstructive pulmonary disease)
- Heavy lifting
If you notice signs of a hernia, like a new bulge, swelling, or discomfort, talk to your healthcare professional. They may recommend changes to your activities, suggest treatment options, or recommend using an ostomy support belt.
Stoma Infection
The first signs of a stoma infection may include pus-like discharge, unusual swelling, increased redness, warmth around the area, a fever, or skin that looks inflamed.
If you think your stoma may be infected, contact your ostomy nurse or doctor before it worsens. Treatment may involve antibiotics, wound care, or changes to your routine.
Ostomy Stoma Necrosis
Stoma necrosis is a rare but very serious kind of ostomy complication. It usually happens soon after surgery, although any major stoma color change should be taken seriously, no matter where you’re at in your ostomy journey.
So what causes stoma necrosis? It occurs when the stoma tissue doesn’t get enough blood flow. A potential warning sign of this is when the stoma changes colors from pink to dark red, purple, blue, gray, brown, or black. The tissue going very pale may also indicate a lack of blood flow or necrosis.
Contact your healthcare professional right away if you notice these signs as quickly as possible, as it indicates tissue death.
Constipation or Output Changes
People with an ileostomy or colostomy may experience changes in ostomy output, including constipation, watery output (diarrhea), or just changes in consistency.
If you have an ileostomy or a colostomy, you may be at a higher risk of constipation or other output changes. This is because the colon absorbs water. Since a portion of the intestines is usually taken out with this type of ostomy, this can lead to dehydration, which in turn can lead to constipation.
If you notice your output is stopping or changing, you may want to reach out to your doctor or ostomy nurse about your options. Sometimes, changing your diet or eliminating certain foods may help.
180 Medical Community member Darlene, who lives with an ileostomy, likes to carry a big bottle of water with her wherever she goes to help support her hydration levels.

Are There Ostomy Supplies That Can Help?
Some stoma problems really need a medical provider’s advice and evaluation. Some require immediate action.
However, some minor issues may improve when your pouching system or skin barrier provides a better fit. For example, frequent leakage, adhesive loosening, or skin irritation may be related to the size, fit, type, or shape of your pouching system. It’s possible some people may benefit from choosing a different ostomy wafer or pouch, or trying ostomy accessories like belts, stoma powder, adhesive remover, or other products.
Your healthcare provider and/or ostomy nurse is the one to go to first to evaluate your problem.
180 Medical’s Ostomy Specialists are here to help you understand what your product options are based on your prescription, insurance coverage, and individual needs.
Find an Ostomy Product Solution For Your Needs
180 Medical’s mission is to provide the best ostomy supplies and caring, personalized service. That means we’re going to treat you like a member of our own family as we work to help you get the products you need.
By choosing 180 Medical, you can get free samples and free shipping. Curious whether your insurance covers ostomy supplies? 180 Medical is in-network with an ever-growing number of insurance plans, including state Medicaid plans, Medicare, and private insurance plans.
Contact us to get started!
Disclaimer: This article is for informational purposes only and is not intended as medical advice. Information provided on 180medical.com should not be used as a substitute for medical advice, diagnosis, or treatment from a qualified healthcare professional. Please consult your healthcare provider with any questions about your condition, treatment, or medical supply needs.